|
Be sensible in your training goals, do not push too hard too quick.Some athletes may choose to go straight to operative fixation if they felt non-operative therapy would be too prolonged but this can be discussed with your surgeon. 
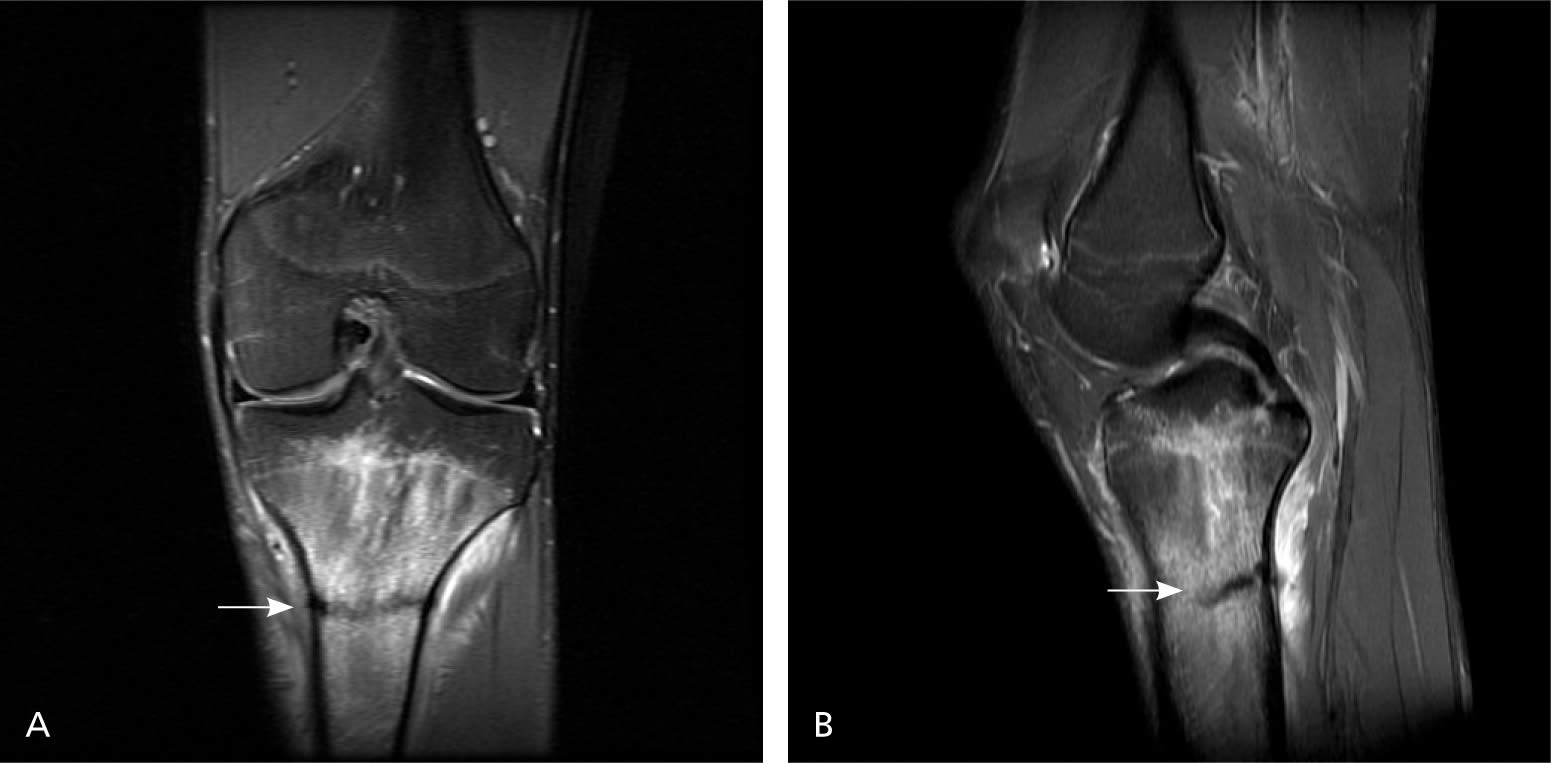
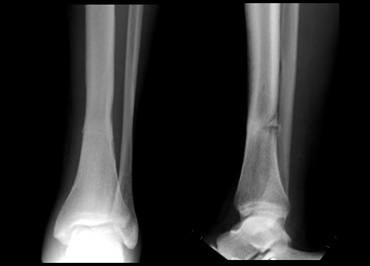
Failing all non-operative treatments may lead to operative stabilisation of the fracture with internal metalwork. If pain continues newer treatments are showing promising results such as shockwave therapy that you can get. If the fracture progresses or activity is instituted too early, prolonged rest is required. Most heal uneventfully between 1 month and 3 months. In the meantime aerobic activity can be maintained by exercise such as swimming, deep-water running and cycling.Īlthough not the rule, but specific injuries where surgery may be advocated early, especially in those athletes wishing to return to sports quickly include: As symptoms resolve training can be gradually re-instituted. Repeated examinations and follow-up MRI scans can check healing. You may be given a plaster cast or rigid boot and crutches. This involves COMPLETE REST FROM RUNNING or activity performed. In general non-operative treatment is usually initiated. The chronic nature of the symptoms, level of activity (professional/amateur), timing during the season and nature of the fracture (displaced or non-displaced, they are usually non-displaced) all dictate the treatment. How is a stress fracture normally treated? A very sensitive test is an MRI scan which nowadays is usually performed to help diagnose some fractures. because it is not uncommon for the X-Ray to show a fracture that looks like it has been “trying to heal” for some time. If an X-Ray shows the stress fracture, patients are often a little shocked when the surgeon says “It looks like that been there for quite a while!”. This depends on duration of the symptoms because if the stress fracture is very fresh or recent then plain X-Rays may not show up anything, until around 3 weeks after the symptoms start. How are stress fractures accurately diagnosed? Commonly statements made to the doctor are “I don’t remember hurting myself” or “I havent really changed my training schedule” or “I thought the ache was nothing to worry about”. Clinical assessment by an Orthopaedic foot and ankle surgeon is advised who has access to multimodal investigation and treatment facilities. Persistent pain in the absence of significant trauma should highlight the possibility of a stress fracture. What should you do if you are concerned you may have a stress fracture? The pain eases on rest but recurs on activity resumption. For example In the tibia or shin, pain radiates on the shin bone on impact, in the 5 th metatarsal pain is located to the outer aspect of the foot, in calcaneum injuries pain is located under the heel. Localised pain in the area of the suspected fracture. This is a combination of disordered eating habits, ammenorhea (absent periods) and osteoporosis (low bone density). There is a classic combination of disorders that can be found even in teenage girls who are keen athletes. Why may women get more stress fractures than men?įemale athletes who suffer from irregular menses (periods) are more likely to develop stress fractures due to the reduced or erratic oestrogen hormone production and the positive effect it has on bone metabolism and strength.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
